Disease Spotlight: Feline Miliary Dermatitis
What is it?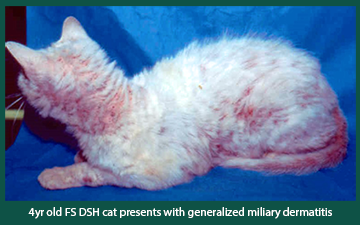
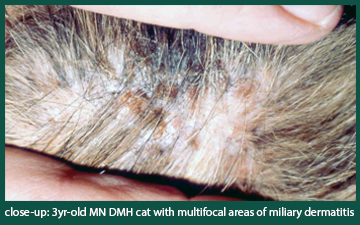
Miliary dermatitis is a unique cutaneous reaction pattern seen only in cats. Clinical signs include crusted papules (bumps) that are often easier to feel than see. Sometimes the crusted papules are edematous (swollen) and exude a clear fluid. The distribution is variable as it can be localized or widespread throughout the haired skin. Pruritus (itch) is variable where the affected feline may or may not also have self-inflicted alopecia (hair loss).
What can cause miliary dermatitis?
 There is a LONG differential list for this unique feline reaction pattern, including: Flea allergy (MOST COMMON), Food allergy, Atopy (pollen allergy), Otodectic mange (ear mites), Cheyletiellosis (superficial skin mite), Trombiculidiasis (chiggers), Notoedric mange (superficial skin mite), Demodectic mange (deep hair follicle mite), Dermatophytosis (ringworm), Staphylococcus folliculitis (superficial bacterial infection), Pediculosis (lice), Ticks, Cat fur mite, Drug eruption, Internal parasitism, Hypereosinophilic syndrome, Biotin deficiency, Fatty acid deficiency, Hormonal deficiency, and idiopathic (unknown).
There is a LONG differential list for this unique feline reaction pattern, including: Flea allergy (MOST COMMON), Food allergy, Atopy (pollen allergy), Otodectic mange (ear mites), Cheyletiellosis (superficial skin mite), Trombiculidiasis (chiggers), Notoedric mange (superficial skin mite), Demodectic mange (deep hair follicle mite), Dermatophytosis (ringworm), Staphylococcus folliculitis (superficial bacterial infection), Pediculosis (lice), Ticks, Cat fur mite, Drug eruption, Internal parasitism, Hypereosinophilic syndrome, Biotin deficiency, Fatty acid deficiency, Hormonal deficiency, and idiopathic (unknown).
How is it diagnosed?
Diagnosis is based on clinical signs and the active search for the underlying cause begins. Diagnostics such as a skin scrape (to look for mites), cytology (to look for bacteria), a ring worm culture, a fecal exam (can be helpful to find mites or mite eggs as ectoparasites are often ingested by the cat), and flea control (THE MOST IMPORTANT, as often fleas are ingested by the cat) are all needed when a cat presents for miliary dermatitis. If more of a work-up is needed: weekly lime sulfur dips, intestinal parasite deworming, antibiotics for several weeks, food trial, intradermal allergy test, complete blood count, discontinue drugs (for a suspect drug reaction), or lastly a biopsy which may or may not help to identify the underlying cause.
What is the treatment?
In order to resolve and prevent the relapse of miliary dermatitis the underlying cause must be identified and treated. In addition, the crusted papules should resolve with the symptomatic therapy of anti-inflammatory doses of steroids (oral or injection). However, steroids are never given until after demodicosis (deep follicular mites), dermatophytosis (ring worm), and pyoderma (bacterial) infections have all been ruled out.
- Feb, 27, 2017
- Disease Spotlight

